Infections of the Central Nervous System
I. Case presentation
A.
Questions
B.
Case notes
C.
More cases
II.
Syndromes of
CNS
infection, causes and treatment
A.
Terminology
B.
Acute bacterial (septic) meningitis
C.
Viral
(aseptic) meningitis
D.
Chronic
meningitis
E.
Encephalitis
F.
Brain abscess
and
empyema
G.
Myelitis and spinal
epidural
abscess
H.
A slide show of
organisms
causing meningitis
III. Lumbar puncture
IV. References
V. Quiz
VI. Abbreviations
VII. About this page
| HOME |
I. Case presentation
Chief complaint: Headache
History of present illness: This is a 35 year old
man with
headache
(1). His headache
began 3 weeks ago,
and has occurred episodically since
then.
It has a pounding quality, is localized to both frontal areas, and is
not
associated with nausea, vomiting, or light-sensitivity. It is relieved
by over-the-counter analgesics. He has had no changes in his vision (2).
The patient has no previous history of similar headaches, and he has no
family history of intractable headaches. He has suffered two episodes
of
impaired consciousness (3).
The
first was two weeks ago; he vomited once, then "passed out" for a few
seconds.
No jerking of the limbs or incontinence was observed. Later, he had a
similar
spell while driving his car.
Past medical history: Hypertension
Physical examination:
Vital Signs T: 97.1
P: 80 R:20 BP: 157/77
General physical exam:
normal. Neck:
supple.
Neurological exam:
MMSE:
28/30. CN: PERRL,
EOMI, visual fields full to confrontation. Visual acuity: OS 20/25; OD
20/30. Funduscopy: bilateral papilledema, L retinal hemorrhage (4).
Motor: normal muscle tone and strength all muscles tested. Sensory:
normal.
DTRs: brisk and symmetrical throughout. Babinski's sign: negative.
Coordination:
normal. Station and gait: normal.
Laboratory studies:
Toxicology screen,
electrolytes,
and ECG were normal. Head CT: normal. Head MRI: no ventricular
enlargement.
EEG: normal.
Course of illness: He
was hospitalized and
the above tests were performed. He was treated with tramadol
(Ultram®)
for pain and amlodipine (Norvasc®) for high blood pressure. A
lumbar
puncture was done: opening pressure was greater than 450 mm of water.
Cell
counts were WBC 213 RBC 46. Differential: segs 1 bands 0 lymphs 81
monos
18. Protein 75. Glucose 24. CSF cryptococcal antigen was positive.
A. Questions
- What are two possible mechanisms of the patient's headache?
- How might the patient's increased intracranial pressure be
treated?
- What is the possible significance of the patient's episodes
of
loss of
consciousness?
- What is the most common fungal infection of the CNS?
- What antibiotic treatments are used for cryptococcal
meningitis?
- What illnesses or therapies predispose to cryptococcal
meningitis?
B. Case notes
(1) Headache
Headache is the most common complaint of patients in a general
neurology
practice. The large majority of headaches are not life-threatening, and
are due to
migraine,
tension, or chronic daily headaches. A small number have serious
underlying
causes: space-occupying intracranial lesions such as neoplasm or
abscess,
subarachnoid hemorrhage, hydrocephalus, meningitis, or encephalitis.
(2)
Headache symptoms
Migraine headache is the most common type of
headache for which
patients seek medical treatment. Diagnosis is purely clinical--there is
no laboratory test. Migraine headache is more common in women than in
men,
and there is often a family history of migraine. The essential symptoms
of migraine headache are severe, throbbing headache with nausea. Other
common symptoms include unilateral headache, photophobia, and
phonophobia.
The patient usually wants to lie down in a dark room, and if she can go
to sleep, feels better on awakening.
In migraine with aura the headache is
preceded by
visual symptoms. This may be as nondescript as vague black spots,
or as dramatic as "scintillating scotoma" or "fortification
spectra"--brightly
colored images with jagged lines. When clearly present, visual symptoms
are invaluable for diagnosing migraine.
Cluster headache is
less common. The pain is nonthrobbing, unilateral, and retroorbital. An
individual headache is brief, but recurs frequently, and the pain is
said to be the most intense of all headache pain.
Tension headache is
very common, but not
usually a cause for visits to the doctor's office. The pain is
moderate,
usually non-throbbing, and tends to be localized to the neck, occiput,
and temples.
Headache pain due to serious causes is
variable.
Most patients with intracranial neoplasm have a
mild headache,
not
usually severe enough to seek medical attention. When present, it has
symptoms
reminiscent of tension headache, but it may worsen at night and awaken
the patient from sleep. Patients with subarachnoid hemorrhage
have
a severe headache of sudden onset, often associated with temporary
confusion
and meningismus. Patients with bacterial meningitis
often have
a
migraine-like headache with severe throbbing, nausea, and photophobia.
Headache in pseudotumor cerebri is variable, but
may have
migraine-like
qualities, and is often associated with transient blurring of vision
that
can, to the unwary, suggest migraine.
(3)
Impaired
consciousness
Sudden onset of impaired or loss of consciousness has two main
causes: syncope
and seizure.
Syncope due to fall
in blood pressure is
most common. It may be preceded by a feeling of lightheadedness, as in
orthostatic hypotension, vasovagal syncope, or vasodepressor syncope,
or
there may be no warning at all, as in sudden ventricular
fibrillation. Onset in vasovagal or vasodepressor syncope is usually
slow, and the
patient
may be able to remember the characteristic symptoms
of lightheadedness followed by blindness prior to
loss of consciousness. When consciousness is lost the patient
collapses
and falls. Usually there is quick recovery once the patient
is
recumbent,
and there is no post-syncope confusion.
The cause of loss of consciousness in
syncope is
global cerebral hypoperfusion--blood pressure drops, so the entire
brain
becomes ischemic for a brief time. Syncope is not due to
primary
brain disease, but if the hypoperfusion is prolonged for more than two
minutes irreversible brain damage begins to occur.
Seizure is also
common. A generalized
tonic-clonic convulsion is usually easy to diagnose from the
history. A complex partial seizure is more difficult to
diagnose.
There often is
a sudden alteration of consciousness, unresponsiveness, often with
purposeless
repetitive behaviors, followed by postictal confusion.
Seizures are caused by the sudden onset
of
paroxysmal
synchronous firing of neurons. Generalized seizures can be a
symptom
of a metabolic abnormality that only secondarily affects
brain. Partial-onset
seizures strongly suggest a specific abnormality of cerebral cortex.
Increased intracranial pressure can
cause syncope
if the increase is large and sudden. Acute hydrocephalus,
such as
may occur with shunt malfunction or intermittent obstruction of the
third
cerebral ventricle due to "ball valve" tumors, may cause
this.
Loss
of consciousness occurs in subarachnoid hemorrhage due to berry
aneurysm
because aneurysmal rupture causes intracranial pressure to temporarily
equal arterial pressure, thereby reducing cerebral perfusion pressure
to
zero.
(4)
Papilledema
and increased intracranial pressure
The rigid skull makes the volume of the intracranial space
constant. The major intracranial contents are:
- Brain parenchyma
- Cerebral spinal fluid
- Blood, venous and arterial
These, like water, are incompressible. An increase in the
volume
of one of these, or the presence of a space-occupying lesion, must
produce
a pressure increase, and will be compensated for by a decrease in the
volume
of one of the other compartments.
Signs and symptoms of
increased intracranial
pressure may include:
- Bulging fontanelle (infants)
- Large head (infants)
- Nausea
- Projectile vomiting
- Headache
- Reduced retinal venous pulsations
- Papilledema
- Cranial nerve VI palsy
- Bradycardia (severe cases)
The headache of increased intracranial
pressure
(ICP)
is not distinctive. Projectile vomiting--sudden forceful
vomiting
without preceding nausea--is distinctive, but not often seen.
The signs of increased intracranial
pressure may
be very helpful for diagnosis. An early and sensitive sign is
venous
engorgement and loss of retinal venous pulsations. When the
pressure
is normal, pulsations can be observed in retinal veins. If
venous
pulsations can be seen, it implies that intracranial pressure is 250 mm
of water or less [21].
Since
pulsations may be difficult to observe, and are absent in 25% of normal
people,
this
sign is more helpful for ruling out high ICP than for demonstrating its
presence.
 |
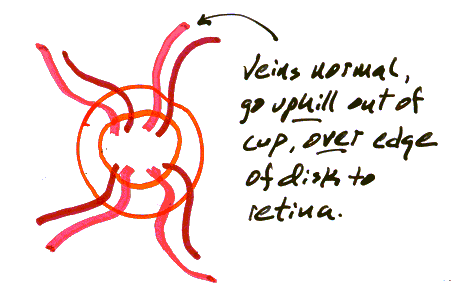
| Figure 1. Venous pulsations |
Venous engorgement and loss of
pulsations occur
because
the central retinal vein drains into the cerebral circulation, so its
pressure
increases when ICP increases.
Papilledema implies swelling of the
optic
disk. Features to look for with the direct ophthalmoscope are:
- Blurring of the optic disk margins, especially the nasal
margin
- Loss of the optic cup
- Engorgement of retinal veins
- Obscuration of vessels passing through the disk margin
- Flame-shaped hemorrhages in the nerve fiber layer
 |
 |
| Figure 2. Normal optic disk |
Figure 3. Papilledema |
Edema of the optic nerve head in
papilledema is
caused
by disruption of fast axoplasmic transport. Axonal material
"piles
up" at the optic nerve head. It is thought that papilledema
can
become
apparent within about six hours of an acute increase in ICP.
Even when its appearance is dramatic,
papilledema
does not produce (initially) diminished vision. If increased
ICP
does cause diminished vision, the increase must have been severe and
chronic,
and a more likely ophthalmoscopic finding is optic atrophy due to
degeneration
of the nerve. In cases in which the optic nerve head is
clearly
swollen,
and vision on the affected side is clearly diminished, a more likely
condition
is papillitis. This may be seen in acute optic neuritis, or
in
anterior
ischemic optic neuropathy. In these conditions the papillitis
is
usually unilateral.
Another non-specific sign of increased
ICP is palsy
of cranial nerve VI. When bilateral cranial nerve VI palsy
occurs
in the absence of other findings, increased ICP is strongly
suggested. The presumed mechanism of cranial nerve VI palsy with
increased ICP is
traction on the nerve. The sixth nerve takes a
long course from its origin at the pontomedullary junction upward over
the wing of the sphenoid bone, and from there to the cavernous sinus.
It may necrose at the point it leaves the subarachnoid space [20].
 |
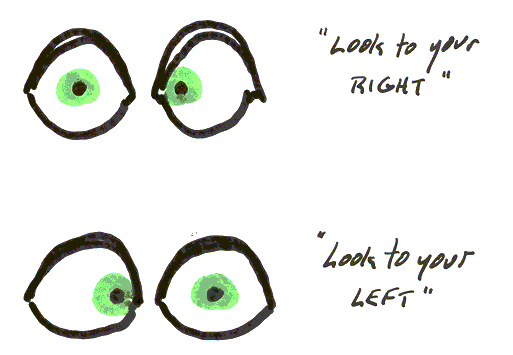 |
| Figure 4. Cranial nerve VI |
Figure 5. Bilateral VIth nerve palsies |
C. More cases
Select a case to study.
- Case 2: an infant with
fever
- Case 3: a man with
headache
II.
Syndromes of CNS
infection,
causes and treatment
A. Terminology
An infection of the central nervous system may primarily affect its
coverings,
which is called meningitis. It may affect the brain
parenchyma,
called encephalitis, or affect the spinal cord,
called myelitis.
A patient may have more than one affected area, and if all are
affected,
the patient has "meningoencephalomyelitis". The
nervous system
may
also suffer from localized pockets of infection. Within the brain or
spinal
cord there may be an abscess, and outside them
there may be an
epidural
abscess or subdural empyema.
B.
Acute
bacterial
(septic) meningitis
Signs and symptoms
- Headache
- Fever
- Meningismus
- Obtundation
Early in the course of the illness, the patient with a purely meningeal
infection will be awake, and painfully aware of his symptoms, so you
may
simply ask him about them. Later in the illness, if untreated, the
meningeal
inflammation will have led to diffuse brain dysfunction, ischemia or
infarction, and
the patient will be stuporous.
The classic signs of meningeal infection
are fever,
stiff neck (meningismus), and headache. Although
characteristic
of
meningitis, headache and meningismus may occur in other infections,
such
as pneumonia. Photophobia, nausea, vomiting, malaise and lethargy are
common.
The latter are also common in "functional" headaches like migraine, and
may confuse the unwary physician.
Meningeal signs
The stiff neck that occurs in meningitis is often striking--it is
really
stiff, almost boardlike, but not so painful as it is stiff. The
stiffness is caused by reflex spasm of the neck muscles due to traction
on
inflamed cervical nerve roots. It is greatest with flexion, less with
extension
or rotation. Of course, a lot of older people have necks that are quite
stiff due to osteoarthritis, and if they have a fever, this may
occasionally
lead to diagnostic concern for meningitis. Usually their necks are
stiff
with both rotational and flexion/extension movement. Associated with
the
stiff neck are two other classic "meningeal signs", the signs of Kernig
and
Brudzinski.
Brudzinski's sign is involuntary flexion of the hip and knee when the
examiner
flexes the patient's neck. Kernig's sign is limitation of straightening
of the leg with the hip flexed. Meningeal signs occur not only in
infectious
meningitis, but in subarachnoid hemorrage and chemical meningitis.
Unfortunately, meningismus occurs only in about 50% of cases of
bacterial meningits, so the sign is neither highly specific nor highly
sensitive.
Diagnosis
- Suspicious clinical symptoms and signs.
- CT of head to rule out abscess or other space-occupying
lesion,
if it
can
be done quickly.
- Lumbar puncture (see below).
- Blood cultures.
Causes and therapy
- S. pneumoniae
- H. influenzae
- L. monocytogenes
- Group B streptococcus
- N. meningitidis
Streptococcus pneumoniae
This organism is now the most common cause of bacterial meningitis
in all age groups except newborns. It is a Gram-positive coccus that
occurs
in pairs (Click
for micrograph [83k]). It has an external polysaccharide
capsule
that
determines its serotype. Serotype is important for vaccine
creation
and epidemiology, but is not routinely performed on clinical isolates,
and does not guide antibiotic therapy.
The nasopharynx is the primary site of
pneumococcal
colonization; 5 to 10% of healthy adults and 20-40% of healthy
children
carry at least one strain of S. pneumoniae, with
higher
incidences
in winter
[7]. Spread is from
person
to person through droplets, so there is an increased chance of spread
in
day care centers, barracks and prisons. It is a serious
illness,
with a case mortality rate of 21% [1].
The organism may spread to the meninges
through
local extension from an infected sinus or middle ear
infection. Because
it colonizes the nasopharynx this strain is common when meningitis
occurs
as a consequence of ENT procedures or of chronic CSF leak.
Major risk factors for meningitis with
this organism
are: splenectomy, diabetes mellitus, liver disease, alcoholism, CSF
leak,
terminal complement deficiency, and pneumococcal pneumonia. Recently,
coclear implant has been found to be a risk factor [22,23].
Treatment and
prevention
For many years, S. pneumoniae was reliably
sensitive to
penicillin. Meningitis caused by these strains responds to meningitis
doses of
penicillin,
ampicillin, cefotaxime, or ceftriaxone.
In recent years, penicillin-resistant
strains have
become common, and these constitute about 30% of cases in Springfield,
Illinois. For the most part these strains remain susceptible
to the
third
generation cephalosporins ceftriaxone and cefotaxime, which enter CSF
in good concentrations [25].
For
meningitis,
a third-generation cephalosporin plus vancomycin is usually recommended
for intial therapy until culture and sensitivity is
available. No
vancomycin-resistant strains have yet been documented, but vancomycin
is
not used alone because of its poor penetration into the CSF. There is
some concern that dexamethasone may reduce blood brain barrier
permeability to antibiotics. Because the organism is sensitive to
rifampin, which easily passes the blood brain barrier, the
addition of rifampin has been suggested [24].
Like pneumococcal pneumonia, meningitis
can be
prevented
with pneumococcal conjugate vaccine. In 2000, routine vaccination of
children with pneumococcal vaccine was begin, but data are not
yet available regarding changes in meningitis incidence.
Hemophilus influenzae
H. influenzae is a small (1-2 micrometer diameter)
Gram-negative
coccobacillus (Click
for micrograph [89k]). Strains causing meningitis
in children
almost all have an outer capsule, but non-meningitis-causing strains do
not.
The organism colonizes the upper
respiratory tract
of humans, who are its only natural host. Spread occurs
through
respiratory
droplets or by direct contact with respiratory secretions. Risk
factors
for meningitis include head trauma, neurosurgery, paranasal sinusitis,
otitis media and CSF leak.
The case fatality rate for meningitis is
approximately
6% [1] in children,
higher in adults.
Treatment and
prevention
H. influenzae meningitis can be prevented by
vaccination. Since the widespread use of H. influenzae
conjugate vaccine
in the 1990s,
the incidence of H.
influenzae meningitis has declined dramatically, with more
than a
90% decline among children under 5 years old [2,3,4,1]. As
with
S. pneumoniae, beta-lactam and ampicillin-resistant
strains
are increasingly found, but resistance to ceftriaxone or cefotaxime are
rare, and these are the drugs of choice.
Rifampin is used for prophylactic
chemotherapy to
prevent secondary cases.
Listeria monocytogenes
Listeria monocytogenes is a facultatively anaerobic
Gram-positive
rod (Click
for micrograph [137k]). The organism can be found in human
feces, unpasteurized milk, cheeses, and other foods. Most cases are
sporadic,
and contaminated food is
the source of infection. It may be difficult to diagnose
clinically,
because compared to other meningitides meningeal signs are less
frequent,
there is a lower CSF WBC count, less neutrophilic predominance, and
lower
protein [5,6].
Cranial nerve
dysfunction
may occur, and there are occasional cases of brainstem encephalitis [26].
Listeria monocytogenes
is a common cause
of meningitis in infants less than 1 month old, and is also common in
adults greater than 60 years old. Risk factors
include
pregnancy,
advanced age, and immunosuppression. The case fatality rate
for L.
monocytogenes meningitis is 15% [1].
Treatment and
prevention
Listeria monocytogenes remains sensitive to
penicillins, and
ampicillin is the antibiotic of choice, but treatment must be
prolonged--3
or 4 weeks. Trimethoprim-sulfamethoxasole is an alternative
for
the
penicillin-allergic patient.
Listeriosis results from food-borne
transmission,
so proper food handling measures markedly reduces infection risk.
Group B streptococcus
This is the most common meningitis in infants less than 1 month of
age (70% of cases) (Click
for micrograph [82k]). Transmission to the neonate
usually
occurs
from mothers colonized by group B streptococcus in the genital
tract. In adults, group B streptococcal infection is often
nosocomial. The
case fatality rate is 7%.
Treatment and
prevention
Beta-lactam-resistant strains of group B streptococcus have not
emerged. Treatment is with penicillin and ampicillin. Neonatal
meningitis
can be prevented by therapies aimed at reducing maternal birth canal
colonization, or by Caesarian section.
Neisseria meningitidis
Neisseria meningitidis is an encapsulated Gram-negative organism that
appears in pairs on Gram stain (Click
for micrograph [80k]). It commonly colonizes the
nasopharynx,
and can spread rapidly from person to person through respiratory
droplets.
N.
meningitidis often occurs in epidemics among persons living
in
close
quarters like dormitories or barracks.
The course of the illness is usually
rapid and
dramatic. Initial non-specific fever, headache, and myalgia give way to
distinctive signs of a petechial rash on the trunk and lower body that
may coalesce
into purpura [fifteen].
Septic shock, disseminated
intravascular
coagulation, and distal extremity necrosis may occur in disseminated
meningococcemia. Although treatment is effective and the
disease
usually
occurs in immunocompetent patients, nevertheless the case fatality rate
is 3% [1]
to 13% [five]. It
is common to
have
non-lethal complications such as cutaneous scars, amputation, hearing
loss,
and renal injury.
As with other encapsulated organisms,
asplenia is
a risk factor for infection.
Treatment and
prevention
Penicillin-resistant strains are uncommon, so drugs of choice are
penicillin
or ampicillin. Ceftriaxone or cefotaxime response is also
excellent. A polysaccharide vaccine has been available for a number of
years and routinely routinely
recommended for all
adolescents,
such as college freshmen or military recruits. It has also
been useful
in patients with risk factors such as asplenia.
Since 2005 a conjugate vaccine has been available [27], which
should now be used instead of the polysaccharide vaccine.
Close contacts of patients have a
significantly
increased risk of contracting infection, so antimicrobial prophylaxis
is
recommended for household members, day care contacts, and
others. This should be done within 24 hours after exposure because
secondary
disease
occurs within several days. For prophylaxis, rifampin is
given
twice
daily for two days, but is contraindicated during pregnancy. One dose
of
ciprofloxacin or ceftriaxone is an alternative, and ceftriaxone can be
given to pregnant patients.
Presumptive therapy for bacterial meningitis
| Age |
Major pathogens |
Antibiotics |
| less
than 3 months |
group
B strep. |
ampicillin |
|
E.
coli |
+
cefotaxime |
|
L.
monocytogenes |
|
|
S.
pneumoniae |
|
| 3 months to 50 years |
S. pneumoniae |
3rd generation cephalosporin (1) |
|
N. meningitidis |
+ vancomycin (2)
|
|
H. influenzae (now rare in USA) |
|
| greater
than 50 years |
S.
pneumoniae |
ampicillin |
or
impaired cellular immunity
|
L.
monocytogenes |
+
3rd generation cephalosporin (3) |
|
Gram
(-) bacilli |
+
vancomycin
|
(1) Ceftriaxone or cefotaxime
(2) Essential in areas with a high prevalence of
penicillin-resistant
S.
pneumoniae.
(3) For patients with penicillin allergy, trimethoprim-sulfamethoxasole
can substitute for ampicillin in treatment of L. monocytogenes.
Pathogen-specific therapy for bacterial meningitis
| Organism |
Drug of choice (1) |
Second choice if allergic |
Duration of therapy |
| group B streptococci |
penicillin G or ampicillin |
vancomycin |
14 - 21 days |
| H. influenzae |
3rd generation cephalosporin |
chloramphenicol |
7 - 10 days |
| L. monocytogenes |
ampicillin + gentamycin |
trimethoprim-sulfamethoxasole |
14 - 21 days |
| N. meningitidis |
penicillin G or ampicillin |
chloramphenicol |
7 - 10 days |
| S. pneumoniae (sensitive) |
penicillin G |
vancomycin + rifampin |
10 -14 days |
| S. pneumoniae (resistant) |
3rd generation cephalosporin + vancomycin |
vancomycin + rifampin |
10 -14 days |
(1) An infectious disease consultatant is always helpful in making
these choices.
Adjuvant therapy
In a recent study of acute bacterial meningitis in adults,
dexamethasone
was shown to significantly reduce morbidity and mortality [19].
Results were best for S. pneumoniae, but no effect
could be
demonstrated
for N. Meningitidis. Dexamethasone has been shown
to reduce
hearing
loss in H. influenzae meningitis [17].
Dexamethasone should be given before or with the first dose of
antibiotic,
at a dose of 10 mg IV every 6 hours for 4 days for adults.
Comments
In meningitis of all kinds there is infiltration of the dura, arachnoid
and pia mater with inflammatory cells. Conveniently, these spill over
into
the cerebrospinal fluid, allowing you to detect them with a lumbar
puncture.
If the condition were to affect only the meninges the condition would
be
bothersome, but no emergency. But that is not the case. Bacterial
meningitis affects brain parenchyma in several ways: release of toxic
bacterial products, stimulation of brain cytokine release, and frank
brain infarction. Some toxic products of S. pneumoniae include
pneumolysin, which forms pores in cell membranes, hydrogen peroxide,
and bacterial cell wall. In the most serious meningitides, brain
infarction occurs. Recall how the
blood supply to brain is from large arteries located in the
subarachnoid
space. These give off small branches that project through the pia mater
at what are called the Virchow-Robin spaces. Meningeal inflammation
affects
these vessels strongly, and the infection can spread to brain itself
through
the Virchow-Robin spaces. In bacterial meningitis this occurs
within
hours, and the condition is curable only if treated early, which makes
bacterial meningitis a
true medical emergency. You can sterilize the CSF at any stage of the
disease,
but you can't heal the brain damage, so the sooner the treatment the
better.
C.
Viral meningitis
Signs and symptoms
- Headache
- Fever
- Viral syndrome
- Meningismus
This is the most common kind of meningitis, and the most
benign. A systemic viral syndrome may be present, but fever and
headache may suggest meningitis. Nuchal rigidity is usually present. It
is highly unusual for focal
neurologic
signs to occur.
Diagnosis
Cerebrospinal fluid usually shows an "aseptic" picture--a lymphocytic
pleocytosis
with dozens to hundreds of WBCs, and normal glucose, protein and
pressure. Viral culture may grow enterovirus, but is usually negative.
Causes and therapy
Enteroviruses are the major pathogens. These include
echovirus,
coxsackie
A and B viruses, and polioviruses. Prior to widespread
vaccination,
mumps was a common cause of this illness. The course
is benign, but the patient may have headache for several
weeks.
Comments
Although uncomfortable, viral meningitis almost never leads to serious
sequelae. However, early in the course of acute bacterial
meningitis
the patient may not be very ill, and the CSF may show only a
lymphocytic
pleocytosis, very much like that of aseptic meningitis [28]. Because
aseptic
meningitis may so closely resemble early acute bacterial meningitis, my
usual tactic is to admit all meningitis patients to hospital for a day
or two of observation, until lack of bacterial growth in CSF
cultures
confirms the meningitis is aseptic.
D.
Chronic meningitis
Signs and symptoms
- Headache
- Fever
- Meningismus
- Confusion
- Hydrocephalus.
In general, symptoms develop slowly. Meningismus may be mild. There may
be subtle mental status changes.
Diagnosis
- This is a difficult diagnosis because signs and symptoms
are
often
non-specific.
It can be suspected in any patient with a chronic encephalopathy, or a
patient with new onset of hydrocephalus.
- MRI or CT of head may show hydrocephalus or contrast
enhancement
of the
basal meninges.
- Lumbar puncture.
Causes
There are a number of causes--bacterial, fungal, parasitic, and
non-infectious.
This is not a complete list, but includes organisms I have at least a
little personal experience with:
Infectious:
- Cryptococcus neoformans (common!)
- Human immunodeficiency virus (HIV)
- M. tuberculosis
- M. avium
- Treponema pallidum
- Nocardia sp.
- Candida sp.
- Aspergillus sp.
- Taenia solium (cysticercosis)
- Brucellosis
- Toxoplasma gondii
Non-infectious:
- Neoplasm (esp. breast, lung)
- Neurosarcoidosis
- Behcet's disease
- CNS vasculitis
- Mollaret's meningitis
Mycobacterium tuberculosis
M. tuberculosis is an acid-fast bacillus. It is
passed
between persons through respiratory droplets. Mycobacteria
multiply
in alveolar spaces or macrophages, and within 2 to 4 weeks hematogenous
spread to extrapulmonary sites occurs. From there, tubercles
develop,
and if brain tubercles rupture into subarachnoid space, meningitis
develops. Deeper tubercles become tuberculomas.
In tuberculous meningitis a thick
exudate forms
and involves blood vessels. Hence, complications of
tuberculous
meningitis
include vasculitis, stroke, and border-zone encephalopathy. Obstruction
to CSF flow may lead to hydrocephalus.
Clinical features of tuberculous
meningitis include
fever, headache, meningismus and mental status changes. Vomiting
and other signs of increased intracranial pressure may occur. Cranial
nerve palsies due to involvement of the basal meninges or increased
intracranial
pressure occurs in approximately 25% of cases. In the U.S.,
HIV
infection
is a risk factor for tuberculous meningitis, and the clinical picture
is
similar. Other mycobacteria (M. avium,
M. africanus)
can produce human disease, and M. avium is an
opportunistic
pathogen
in AIDS patients.
Spinal cord may be involved by
tuberculosis. Usually the thoracic cord is affected, and syringomyelia
can be a late
effect. Tuberculous spondylitis may result in a psoas abscess
or
an epidural abscess.
Cerebrospinal fluid
The CSF in tuberculous meningitis shows a lymphocytic pleocytosis with
elevated protein and reduced glucose. Staining for
mycobacteria
is
positive in 5 to 25%, and culture is positive in approximately 60% of
cases. In some cases as many as four CSF examinations may be required
to
detect
the organism, or it may be necessary to sample directly from
ventricular
fluid. CSF PCR may be useful.
With treatment, the CSF returns to
normal
slowly. Glucose is the first to normalize, but it takes at least three
weeks,
and
usually more [8].
Imaging
Contrast-enhanced CT or MRI scans show a basilar meningitis, with
contrast
enhancement of the meninges in the suprasellar area, prepontine
cistern,
or interpeduncular fossa. Obstructive or communicating
hydrocephalus
may occur.
Therapy
Therapy is prolonged--isoniazid,
rifampin and
pyrazinamide
daily for two months, then isoniazid and rifampin daily or twice weekly
for four months [9].
Therapy may
be
even longer in patients who show a slow response.
There is evidence that corticosteroids
improve
neurologic
outcome [10].
Prognosis and
complications
Death occurs in 25% of cases. Complications of the disease
include
brain infarction in 25 to 40% due to involvement of perforating vessels
at the base of brain. Infarction of the basal ganglia is
especially
common. Hyponatremia due to hypothalamic involvement may also
occur.
Fungal infections
Depending on growth conditions, dimorphic fungi exist in a yeast
(unicellular)
form or in a filamentous (mold) form. In the filamentous form
they
have tubular structures called hyphae, which are divided into
segments. Some segments have the ability to form spores.
Most fungal infections begin with
inhalation of
spores, but may also come from indwelling catheters, mouth or GI tract
(Candida), nasal sinuses (Aspergillus
sp., Zygomycetes
sp.) or skin (sporotrichosis).
The most common organisms in CNS fungal
infections
are Cryptococcus neoformans (Click
for micrographs [121k and 82k]), Coccidioides
immitis, Histoplasma
capsulatum, and Blastomycetes dermatididis.
The clinical
presentation
is usually as a subacute or chronic meningitis, but fungal abscesses
may
also occur and cause focal neurologic signs.
Risk factors include AIDS (Cryptococcus),
organ transplantation or diabetes (Aspergillus),
or
indwelling
intravascular catheters (Candida). The
likelihood of CNS
disease
is increased in the presence of systemic disease of kidney, lungs, or
skin.
Cerebrospinal fluid
The white blood cell count is usually moderately elevated, with 20
to 1000 cells per cu. mm. Lymphocytes usually predominate. Aspergillus,
Blastomycetes,
and Zygomycetes may cause a neutrophilic
predominance, and Coccidioides
may cause eosinophils to occur in the CSF. Special stains for
fungi
may demonstrate the organism.
Cryptococcus
neoformans, in addition to
being
the most common fungal meningitis, is the easiest to diagnose in the
laboratory.
CSF culture for this organism, although growth is slow, is usually
positive. For cryptococcus, a sensitive and specific test to detect
capsular
antigen
is available and can be performed rapidly, so it is quite useful for
clinical
management. For initial diagnosis, test of the antigen in the
CSF
is most useful, but serum tests can be useful for following the course
of therapy. The India ink test for cryptococcus, although quite
specific,
is not very sensitive, and no longer routinely performed by some
laboratories.
Antigen tests are not available for
other
fungi. Antibody tests are available, but immunosuppressed patients may
not be
able to mount a significant antibody response. PCR is not yet
clinically
available.
Diagnosis
With Cryptococcus, diagnosis can usually be made
from CSF
studies. With other fungi, recovery of the organism from a non-CNS site
such as
skin, joint fluid, lung lesions, sinuses, bone marrow, urine, or blood
is helpful. Often, brain biopsy is required. A
diagnosis
based
on cultures from other body sites must be considered probable rather
than
definite.
Treatment
The drug of choice for all fungal meningitides is amphotericin B, but
it has several disadvantages. It must be given intravenously
rather
than PO because of poor gut absorption. It can be given
intrathecally,
but discomfort and toxicity are considerable with this route. It
crosses the blood-brain barrier poorly and the dose that can be given
is
limited by renal toxicity. Intravenous doses cause a variety
of
unpleasant
side effects including fever, chills, nausea, and vomiting, but
adjunctive
medications (diphenhydramine, ibuprofen, prochlorperazine) are used to
control these symptoms. Life-threatening, but uncommon
reactions
include anaphylaxis, seizures, and cardiac effects. Drug
treatment
may have to be halted if rises in serum creatinine indicate renal
toxicity. New lipid formulations of amphotericin B may reduce these
toxicities.
Fluconazole is also useful, and it can
be given
by mouth as well as intravenously, but the cure rate is lower than with
amphotericin B. Fluconazole is standard for AIDS patients
after a
course of amphotericin is finished. Patients with C.
neoformans,
Candida
sp., or
Aspergillus sp. may also be given flucytosine,
especially
if the patient has AIDS.
Complications
Half or more of patients with fungal meningitis develop
complications. Communicating hydrocephalus is common (5 to
10% with
cryptococcal
meningitis), and may result either from blockage of CSF flow within the
basal cisterns, or in the arachnoid villi of the sagittal
sinus. Arachnoiditis can cause obstructive hydrocephalus by blocking
outflow
from
the IVth ventricle. Stroke, cranial nerve palsies, seizures,
and
encephalopathy can also occur.
Other causes of chronic meningitis
- Syphilis. Caused by
a spirochete, Treponema
pallidum,
CNS syphilis is a very rare cause of meningitis in the penicillin
era. If CNS syphilis is a concern, a CSF VDRL should be checked.
- Lyme disease. Lyme disease
is rare in central
Illinois, and
Lyme meningitis or encephalitis is even rarer.
- Cysticerchosis. A parasitic
infection of brain,
this
is the
most common cause of epilepsy worldwide, but is rather rare in the U.S.
The diagnosis is usually first suspected when multiple cysticerci are
detected
on brain imaging studies.
- Carcinomatous meningitis. This
is associated with
neoplasm
such as breast cancer or lung cancer. It is uncommon, but not
rare. Diagnosis requires a high index of suspicion, and is confirmed by
finding
malignant cells in CSF with cytologic examination.
E. Encephalitis
Symptoms and signs
- Confusion
- Personality change
- Altered mental status
- Fever
- Seizures
The patient with encephalitis is having problems with his brain, and
likely
with thinking, so he may not give you a good history. Family and
friends
may report the characteristic symptoms: personality change, lethargy,
confusion,
irritability. Focal neurologic signs are uncommon. The time course may
be short in case of herpes simplex encephalitis (days), or much longer
as in the case of Creutzfeld-Jakob disease (months). The only common
acute
encephalitis that is caused by herpes simplex virus. Its time course is
relatively short, and fever, altered mental status and seizures are
common.
A triad of symptoms that should definitely bring it to mind is: fever,
personality change, seizures. The only common chronic
encephalitis
in Illinois is HIV encephalitis.
Diagnosis
- History and physical
- Brain imaging to rule out space occupying lesion
- Lumbar puncture
- Culture of CSF (some organisms)
- Acute and convalescent titers of antibody
- PCR of CSF for Herpes encephalitits
- Brain biopsy in exceptional cases
Causes
- Herpes simplex viruses
- Varicella zoster virus
- Human immunodeficiency virus
- Rabies virus
- Many others
Herpes simplex virus
By far the most common sporadically-occuring encephalitis is that
caused
by herpes simplex virus (HSV). HSV-1 (herpes labialis)
is
most common in adults, with only 6 to 15% of cases caused by HSV-2
(genital
herpes) [11], but
HSV-2 is more common
in
neonates, who are infected by passing through mother's infected birth
canal.
Primary HSV-1 infection usually occurs
in the mouth,
and is asymptomatic. Symptoms later occur with painful
lesions on
the mucosa of the cheek or gums. After primary infection the
virus
establishes a latent infection in the trigeminal ganglion. Encephalitis
may occur either during the primary infection or during reactivation of
a latent infection.
The clinical presentation includes
fever, headache,
and behavioral abnormalities or personality changes. Seizures
and
focal neurologic deficits often occur. Initial symptoms may be mild, so
several days may elapse before the seriousness of the illness becomes
apparent.
HSV-1 encephalitis causes inflammation
and necrosis
in the temporal lobes and frontal cortex, which easily explains the
tendency
to cause seizures, personality change, and neurologic deficits.
Diagnosis
MRI of the head shows T2-bright lesions in the medial and inferior
temporal lobes. EEG may show nonspecific slowing, or may show
periodic
discharges in the temporal leads on one or both sides.
CSF examination may show an increased
opening
pressure
if there is significant brain swelling. There usually is a
lymphocytic
pleocytosis of 5 to 500 cells per cu. mm and a mildly elevated
protein. Red cells and xanthochromia are usually present. CSF viral
cultures are
usually negative. PCR of CSF to detect HSV nucleic acid is
useful,
though in our laboratory the result returns too slowly to be useful in
deciding whether to use antiviral therapy. In addition, the
reaction
is inhibited by RBCs, so false negative results can occur.
Brain biopsy demonstrates Cowdry A
intracellular
inclusions, and is relatively sensitive and specific for the condition,
but is not usually performed if a probable diagnosis can be made
without
it.
Treatment and
prevention
Intravenous acyclovir (10 mg/kg every 8 hours for 2-3 weeks) is
standard. Rarely, HSV is resistant to acyclovir, and must be treated
with
foscarnet
[12]. Neonatal HSV-2
encephalitis can be prevented by Caesarean section.
Arthropod-borne encephalitis
West Nile Virus [18]
The West Nile Virus (WNV) first appeared in the U.S. in New York in
1999, and has since spread nationwide. In 2002, Illinois had the
distinction
of being the state with the most cases of WNV. In 2002 WNV was by far
the
most common etiology of viral encephalitis in the state. WNV's natural
host is birds, especially crows and blue jays, and these animals
develop
a high titer viremia. It is transmitted from viremic birds to humans by
Culex
mosquitoes. Humans develop only low-level viremia, and human-to-human
transmission
by mosquitoes has not been documented. A few cases have been documented
of WNV transmitted by blood transfusion, organ transplantation, breast
feeding, by placental transmission, or by exposure of laboratory
workers
to infected sera or animals.
The viral incubation period is 2 to 15
days. Most
patients have an asymptomatic infection, but 20% will develop a fever,
headache, backache, myalgia, and anorexia, lasting 3 to 6 days. About
50%
develop a rash, and lympadenopathy can occur. About 1 in 150 infections
will cause a severe illness with meningoencephalitis. Age is a strong
risk
factor, with the risk for 80 year olds almost 50-fold increased.
Symptoms
include flaccid weakness due to involvment of anterior horn cells, or
less
commonly parkinsonism, ataxia, polyradiculopathy, seizures, and cranial
neuropathy. Mortality of the neurologic illness is about 10%, and
recovery
is rather poor in non-fatal cases.
Radiologic findings are nonspecific.
Diagnosis is
based on clinical history, serology, and CSF findings. CSF shows a mild
pleocytosis (30 - 100 cells/mm3), primarily lymphocytes, mild protein
elevation,
and normal glucose. Serologic tests are perfomed on both serum and CSF.
WNV IgM is detectable in 90% of patients at 8 days, and persists for
more
than 6 months, so it is not an indicator of an acute infection. WNV IgM
in the CSF indicates CNS infection. IgG antibodies increase between
days
7 and 21.
There is no specific treatment.
Prevention relies
on mosquito avoidance and control.
Other arbovirides
The most common in the midwest U.S. are La Crosse virus and St. Louis
encephalitis. They are transmitted by mosquitos and occur
mainly
in late summer and early fall. Symptoms are those of a
flu-like
illness,
with evidence of brain involvement indicated by lethargy, confusion,
irritability,
tremors, or seizures. La Crosse virus may produce focal
neurologic
signs. St. Louis encephalitis may be associated with
hyponatremia
due to SIADH.
CSF shows a lymphocytic
pleocytosis. Diagnosis
requires a fourfold rise in antibody titer between acute and
convalescent
sera, viral isolation from CSF, or demonstration of IgM antibody in
CSF.
Treatment is merely supportive--no
specific
antiviral
therapy is available.
Other causes of encephalitis
Primary infection of meninges or brain by human immunodeficiency virus
(HIV) is common, and causes meningitis or encephalopathy.
Rabies
virus encephalitis is very rare, and almost invariably fatal. It
can be prevented by immunization after exposure to a rabies-infected
animal. In the immunosuppressed patient, varicella-zoster virus,
Epstein-Barr
virus,
human herpes virus type 6, cytomegalovirus, measles and enterovirus can
all occasionally cause encephalitis.
Therapy
- For herpes simplex encephalitis, intravenous acyclovir is
curative.
- Varicella-zoster encephalitis can be treated with
intravenous
acyclovir.
- For HIV encephalitis, treatment for HIV is continued, but
there
is no
specific
treatment for the nervous system involvement by the virus.
- CMV encephalitis can be treated with ganciclovir.
- Rabies encephalitis can be prevented by vaccination after
exposure to
the
rabies virus, but once the encephalitis has begun there is no effective
treatment and death is practically certain.
Comments
HSV is the most common cause of sporadic encephalitis. An
effective,
safe treatment for it exists, but not for other infections, so many
patients
with encephalitis are treated presumptively with acyclovir.
F. Brain
abscess and empyema
Brain Abscess
Symptoms and signs
- Headache
- Focal neurologic deficits
- Fever, chills and other signs of infection usually do not
occur
- Papilledema (with increased ICP)
- Nausea, vomiting (with increased ICP)
Diagnosis
- Focal neurologic deficit or seizure suggests focal brain
lesion
- The patient may have a risk factor for abscess, such as:
- congenital heart disease with right to left shunt
- bacterial endocarditis
- lung abscess or bronchiectasis
- paranasal sinusitis
- Contrast-enhanced CT or MRI may show a ring-enhancing
lesion or
lesions
and surrounding brain edema
- If the diagnosis is in doubt, a stereotaxic brain biopsy
will
confirm
that
the lesion is an abscess
Cerebrospinal fluid
Lumbar puncture is not usually performed because abscess creates an
intracranial
mass with edema, so there is a risk of brain herniation. If
the
abscess
is well-encapsulated, protein may be increased, but cell counts are
usually
low and cultures are usually negative, so the diagnostic usefulness of
LP is limited even if the physician is bold enough to do it.
Treatment
If the abscess is small and not causing severe neurologic deficit,
presumptive
antibiotic therapy can be given--usually a combination regimen that
covers
both aerobic and anaerobic organisms is needed. If the
abscess
grows
or fails to resolve, then surgery will be needed for diagnosis and
drainage.
Etiology
Abscesses may arise by spread from an intracranial infection such as
mastoiditis,
but usually are spread to brain through the blood stream. Hematogenous
spread from heart or lungs is most common. Congential heart
disease
with right to left shunting, pulmonary A-V fistulas, bronchiectasis,
and
lung abscess are all risk factors. Bacterial endocarditis is
usually
only a minor risk factor for brain abscess.
Streptococcus viridans
is the most commonly
isolated organism, but abscesses are usually polymicrobial, and Staphylococcus
aureus, hemolytic Streptococcus, Enterobacteriaciae,
Bacteroides
and other anaeobes, are also common. In immunocompromised
patients,
fungal or Toxoplasma gondii abscesses may occur.
Subdural empyema
Subdural empyema is a collection of pus in the subdural space, usually
arising by direct spread from an intracranial infection such as
sinusitis. Signs and symptoms are like those of brain abscess, but
seizures are
especially
common, and treatment essentially always requires surgical drainage.
G. Myelitis and
spinal epidural abscess
Symptoms
- Fever
- Back pain
- Limb weakness or sensory changes
- Bowel or bladder dysfunction
Symptoms are those of spinal cord dysfunction: weakness, sensory
changes, bladder or bowel dysfunction. In the case of epidural abscess,
localized back pain and fever are very common.
Signs
Signs are those of spinal cord dysfunction: paraparesis, sensory level,
hyporeflexia or hyperreflexia with extensor plantar responses, loss of
anal reflexes, loss of anal tone and loss of bulbocavernosus reflex.
Diagnosis
- Characteristic signs and symptoms.
- MRI of the spine at the level suggested by the clinical
exam.
- Lumbar puncture for suspected myelitis, but not for spinal
epidural
abscess.
Causes
Myelitis may occur along with meningeal or brain infection, but often
occurs
alone, causing a syndrome of acute transverse myelitis. Acute
transverse
myelitis is characterized by the rapid onset of spinal cord
dysfunction,
without evidence for spinal cord compression or infarction. CSF
pleocytosis
occurs. It is usually thought to be of viral etiology.
Spinal epidural abscess also produces a
rapid-onset
spinal cord syndrome. The most common cause is S. aureus.
LP is contraindicated in spinal epidural abscess because: 1) by
needling
the abscess you may seed the CSF with bacteria, causing a meningitis,
2)
you may precipitate spinal block, with immediate complete paraplegia.
Therapy
Therapy for acute transverse myelitis is mainly just supportive, but
treatment
with high dose steroids is worth considering. Spinal epidural
abscess
is a medical emergency because loss of function can be prevented by
prompt
surgical drainage of the abscess, but if diagnosis or treatment is
delayed
until paraplegia occurs, recovery is very poor. Appropriate antibiotic
therapy is essential.
Comments
Myelitis is usually caused by viral organisms. I usually treat it with
steroids, but the results are usually unsatisfactory. Epidural abscess
is uncommon, but not rare. It is a true medical emergency--if you
diagnose
the abscess, drain it, and treat with antibiotics before it causes
severe
spinal cord symptoms your patient will be able to walk out of the
hospital.
If you mistakenly believe it is something you can work up and treat at
a leisurely pace, your patient will probably leave in a wheelchair.
H. A slide show
of organisms causing
meningitis
 |
This is a "Rogues Gallery" of microscopic images of
organisms
that
cause meningitis. Images are courtesy of Dr. Joan Barenfanger.
|
III.
Lumbar puncture
Lumbar puncture is essential for diagnosis in most cases of meningitis
and encephalitis (but not for abscess or empyema). The test is
sensitive
and specific for most organisms.
How to do it
- Position the patient. (This is like chess--position is half
the
battle.)
- Place the patient in the left lateral decubitus position
with his
back
toward you. (That is, lying on his left side, with his head to your
left.)
- Have the patient curl up into a ball, chin trying to touch
the
chest,
knees
pulled up to the chest. This tends to separate the spinous processes,
and
make it easier to get in. ("Arch your back like a mad cat!")
- Identify the L3/4 interspace. First, find the middle of the
spine,
marked
by the spinous processes. The spinous processes stick out a little and
are hard like bone. The interspaces are softer. Palpate the
posterior
superior iliac crest (the top of the pelvis). The L3/4 interspace is
the
one crossed by a perpendicular line dropped from the posterior superior
iliac crest.
- Mark that space. I use a ballpoint pen to make lines on
either
side of
it, pointing to it. (I don't want to introduce ballpoint ink
into
the CSF).
- Open the LP tray, put on your gloves, and perform a sterile
prep
and
drape
of the patient. This is extremely important but difficult to describe
in
words so I won't--observe the procedure once or twice, then do it
yourself
under supervision. Some people think that they don't need to use a
drape,
but I strongly advise that you do; it's just too easy to contaminate
yourself
without it, and if you have draped the patient, you can feel for
landmarks
like the iliac crest without breaking sterility.
- Prepare the kit. You'll need to set up a manometer to
measure the
pressure,
and you'll have to loosen the caps of the tubes so that you can
manipulate
them with one hand. Keep the caps loosely over the tubes, so that if
your
assistant coughs it doesn't contaminate your sample.
- Ask the patient if they have an allergy to local
anesthetics. If
not,
then
anesthetize the interspace with 1% lidocaine. Make sure the air is out
of the syringe, and if you anesthetize deeply, try withdrawing before
you
inject to make sure you're not in a vessel. I anesthetize
just
the
skin, and try to raise a orange-peel-like bleb with the anesthetic to
ensure
I get the epidermis, which is most pain-sensitive layer. Many
physicians
use a longer needle to anesthetize deeply, but I don't--I don't think
it
spares the patient any pain. If they are allergic to
anesthetics,
then I do it without anesthesia.
- Take the spinal needle, and orient it this way: bevel
upward (to
split,
rather than cut, the fibers of the posterior longitudinal ligament);
precisely
perpendicular to the patient's back in a vertical direction; aim toward
the patient's navel.
- Push the needle in. Don't try to be slow and "gentle"--it
just
hurts
more
to go slowly. If you hit bone, back up all the way to the
skin
and
aim again. You may have to do this more than once. As you go through
the
posterior longitudinal ligament you sometimes feel a slight pop. If
you
think you may be in the thecal sac, pull out the stylet and see if you
get CSF flowing out. If not, put the stylet back in and try again. You
will often get blood return, because the thecal sac is surrounded by an
extensive venous plexus. If blood clots in your needle you
will
need
a new one. If the patient complains of back pain--well,
there's
nothing
to do but reassure them it will be over soon. If the patient complains
of pain in the hip or leg, ask them which one, because you are touching
a spinal nerve root. If the pain is on the left side, your needle may
be
aimed too far down and you'll need to re-aim. If the right side, then
you're
too far up.
- Got fluid? If the fluid is bloody, waste the first 3 or 4
drops
so that
a bloody tap doesn't confuse you. Measure the opening pressure with
your
manometer. Collect approximately 2 cc of fluid in each tube for the
usual
diagnostic tests. If you want to culture for tuberculosis or fungi,
collect
10 cc in one tube. If you want to test for abnormal cytology, then the
more the better, but get at least 10 cc for the cytology alone.
- Done? Put the stylet back in, then withdraw. (Neurologic
legend
says
you
may vacuum up a nerve root with your needle if you don't put the stylet
back in.)
- Having trouble? Try the L2/3 space.
- Still having trouble? Try sitting the patient up to do
it--the
interspaces
may separate better and the lumbar CSF pressure will be higher.
- Still having trouble? Better ask a
radiologist to do it
under fluoroscopic
guidance. If you possibly can, go watch the procedure so you can
understand
the anatomy better.
Looking at the sample with the naked eye
Immediately upon obtaining the sample, it may be obvious that it is
bloody
or cloudy. In bacterial meningitis it is common to have thick
cloudy
fluid, usually implying a cell count in the thousands. In
subarachnoid
hemorrhage the fluid is frankly bloody, but it must be distinguished
from
merely a "traumatic tap". If the fluid becomes clear during
the
procedure,
traumatic tap is likely.
If the fluid looks normal with casual
observation
it could still be abnormal to the expert observer, who may detect
xanthochromia. Xanthochromia is a yellowish or reddish discoloration of
the spinal
fluid
caused by pigments resulting from breakdown of red blood
cells. To
test for it, the fluid should first be centrifuged to sediment out
cells.
In severe cases, the spun fluid may look like cherry
"Kool-Aid". More subtle cases can be detected by holding the tube up to
a window
illuminated
by sunlight. (Personally, I prefer the bright northern light
of a
cloudy winter day, but in a pinch a 5500 K halogen lamp will
do.)
Observe the fluid for a yellowish tinge. If there are
refractile
particles, you didn't spin it long enough--these are WBCs or RBCs.
Looking at the sample with a microscope
Cell counts
Three pieces of equipment are required: a microscope, a hemocytometer,
and coverslips of a weight appropriate for the hemocytometer. To
do a cell count, place the coverslip on the hemocytometer, then place a
drop of CSF in the well of the hemocytometer. The drop will
be
drawn
under the coverslip by capillary action.
The field of the hemocytometer will have
nine
subdivisions,
and the central one will be further subdivided. The total
volume
under the slip is 0.9 cubic mm. If there are lots of cells,
count
the cells in one large square and multiply by 10 to get the total
number
of cells per cubic mm. If there are few cells, count all 9
squares.
This technique will allow you to quickly obtain a count of total RBCs
and
WBCs, and will allow you to examine RBC morphology. If the
RBCs
are
round, they are fresh, and likely are there because of a traumatic
tap. If they are crenated (wrinkled), they are likely to have been in
the
CSF
prior to the procedure.
Gram stain
For the truly devoted student of CSF, doing your own Gram stain is
a must. For this, you will need, in addition to a microscope,
a
sink
with running water, gloves, and the necessary staining
paraphernalia. Instructions on this can be found elsewhere.
Tests to run on the sample
It is standard to obtain four tubes of CSF, each containing 1 or 2 cc
of
fluid. Standard tests include:
Tube #1: glucose and protein
Tube #2: cryptococcal antigen, Gram stain
Tube #3: bacterial cultures
Tube #4: cell count and differential
Glucose
CSF glucose is normally 2/3 that of the serum. Hence, for an
accurate assessment, a simultaneous serum glucose is
necessary.
Glucose
is normal in viral meningitis, and may be normal in chronic meningitis,
but is often very low in acute bacterial meningitis.
Protein
Protein is increased in any condition in which a leaky blood brain
barrier occurs. Hence, it is increased in conditions
affecting
the
spinal nerve roots (diabetes, Guillian-Barre syndrome), may be
increased
in neoplasms of the CNS, or infections of the brain, spinal cord, or
meninges. Protein may be markedly elevated in cases of spinal block
(for example,
severe cervical stenosis or neoplasm), but LP is contraindicated in
patients
with these conditions because of the risk of producing spinal cord
compression. Protein is also increased with normal aging--a rule of
thumb is that a
person is "allowed" 1 mg/ml of protein per year of age.
In case of traumatic tap, protein is
increased
because
of the inclusion of cells and serum in the sample. A rule of
thumb
is that 1000 cells imply a 1 mg/ml increase in protein
concentration. If accuracy is imperative, then the amount of protein to
be expected
can
be calculated if the patient's serum protein concentration, RBC counts,
and WBC counts are known.
WBC count
This is a critical number in cases of meningitis. The
meninges
are everywhere close to the spinal fluid spaces, and early in the
course
of illness, inflammatory cells spill from the meninges into the
CSF. The WBC count is normally 5/cu. mm or less. It is increased
into
the tens and hundreds or thousands by septic meningitis.
The differential can help in determining
the type
of infection. In aseptic meningitis, mononuclear forms,
especially
lymphocytes, predominate. In septic meningitis,
polymorphonuclear
forms predominate. If the overall count is normal the
differential
is not meaningful.
A number of non-infectious conditions
can produce
small increases in CSF WBC counts, including:
- Seizures. Cell counts of 25 or so are
common immediately
after a
generalized seizure.
- Multiple sclerosis. During an acute
exacerbation, cell
counts in
the dozens are common.
- Stroke. Stroke, especially embolic
stroke, may be
associated
with
cell counts in the dozens. This is even more likely if the
stroke
is caused by bacterial endocarditis.
RBC count
This is increased in subarachnoid hemorrhage and traumatic
tap. The RBC morphology may be helpful--if they are crenated they are
likely
to have been present in the CSF for some time, and not caused merely by
the trauma of the procedure (unless the specimen is allowed to sit on
the
desk of a ward clerk or a laboratory technician for a long time before
it is examined).
Bacterial cultures
Cultures are the "gold standard" for diagnosis of bacterial
meningitis. Normal CSF is always sterile, so if cultures grow the
patient either
has
an infection, or the specimen was contaminated. In bacterial
meningitis,
cultures are positive in the large majority of cases: 80% for S.
pneumoniae,
90% for N. meningitidis, 94% for H.
influenzae. False-positive
results occur if the culture is contaminated by skin organisms such as
coagulase-negative
staphylococcus, but this organism often is
the infectious agent in cases of shunt infection. False-negative
results are often obtained if the meningitis has been partially treated
with antibiotics before the CSF specimen is obtained.
It is worth noting that patients with
meningitis
are often also bacteremic, so blood cultures are usually positive as
well.
A drawback of CSF cultures is that it
takes 24 to
48 hours for the organism to grow and be identified.
Gram stain
Gram stain is an essential part of the CSF examination whenever
meningitis
is considered. In addition to being practically 100%
specific, it
has a sensitivity of 60 to 80% for bacterial infection [13,14].
Bacterial
antigen tests
Rapid bacterial antigen tests are available for S. pneumoniae, N.
meningitidis, and H. influenzae.
Other tests
Other tests may be useful in particular clinical situations:
- Traumatic tap. Do cell counts
on tubes #1 and #4.
If the
RBC
count goes down significantly, traumatic tap is likely.
- Chronic meningitis. Add a
VDRL to check for
syphilis,
an acid-fast
bacillus stain for M. tuberculosis, and fungal
cultures.
- Multiple sclerosis. Collect
10 cc for CSF
electrophoresis
to detect the characteristic oligoclonal bands.
- Carcinomatous meningitis. Collect
as much CSF as
possible
for cytologic examination. The more CSF is available, the
more
likely
it is that the spun-down specimen will contain malignant cells.
- Pseudotumor cerebri. No
further tests on the fluid
are
required,
but the clinician may want to obtain large amounts of fluid to lower
the
pressure, measure a closing pressure to ensure that the pressure has
been
decreased, and determine whether the procedure provides relief from
headache.
- Aseptic meningitis. Viral
cultures are worthwhile
when
positive,
but detect less than 25% of cases [15,16].
Acute and convalescent antibody titers in the serum may be useful.
- Encephalitis. The most common
organism is herpes
simplex. CSF PCR may be useful for confirmation of the diagnosis, but
in my area at the
time
of this writing the test cannot be obtained rapidly enough to use a
negative
result to select patients who needn't be treated with acyclovir--so
clinical
diagnosis is still paramount. PCR is available for HSV I,
CMV,
VSV,
EBV and enterovirus, and has a sensitivity and specificity of 90-100%
in
each. Consider
ordering a viral culture as well--although it is usually
negative,
it may become positive before the PCR result returns from the lab you
sent it to.
Typical CSF formulas
|
Bacterial |
Viral |
Fungal |
Tuberculous |
| opening pressure |
normal or high |
normal |
normal or high |
usually high |
| WBC count (cells/mm3) |
1,000-10,000 |
< 300 |
20-500 |
50-500 |
| PMN (%) |
>80 |
<20 |
<50 |
~20 |
| mononuclear forms |
|
lymphocytes |
|
|
| RBC count (cells/mm3) |
slight increase |
normal |
normal |
normal |
| protein (mg/dl) |
very high (100-500) |
normal |
high |
high |
| glucose |
< 40 |
normal |
usually < 40 |
< 40 |
| Gram stain |
60-90 % positive |
negative |
negative |
AFB stain + in 40-80% |
| culture (% positive) |
70-85 |
25 |
25-50 |
50-80 |
Relative contraindications to lumbar puncture
- Space-occupying intracranial lesions or
obstructive
hydrocephalus.
The risk is that removing fluid from the lumbar space would exacerbate
a pressure differential between intracranial compartments and lead to
brain
herniation. This is uncommon, but is a definite concern. Careful
examination
of the patient for signs of increased intracranial pressure (e.g.
papilledema)
is indicated. An emergency non-contrast CT scan of the head is also
indicated.
If a scan is not immediately available, your choice is between (a)
presumptive
treatment and no lumbar puncture, or (b) puncture without scan. Either
may be the most reasonable depending on the clinical situation. Brain
absess
is thought to be especially likely to be associated with herniation.
Papilledema
and increased intracranial pressure are not by themselves a
contraindication
to LP. In fact, LP is a good therapy for the increased intracranial
pressure
of pseudotumor cerebri.
- Bleeding dyscrasia. If necessary, give
two units of
fresh
frozen
plasma and do the LP right away. But the risk of serious complication
here
is low, so do not delay long if you suspect bacterial meningitis--the
two
hours you delay may mean the difference between a normal life or a
brain-damaged
one.
- Spinal epidural abscess. Do not put a
lumbar puncture
needle
through
the abscess--you may seed the subarachnoid space with bacteria and
cause
a meningitis.
Possible complications
- Headache. Occurs in 20% of patients,
caused by leakage
of
fluid
through the hole made in the dura. Diagnosis is obvious--the
headache
is severe when standing but immediately goes away on lying down.
Treatment
is bedrest with the head lower than the hole, and drink plenty of
fluids.
- Meningitis. Rare. Should occur only if
there is some
break
in sterile
technique--which is to say it should never occur.
- Contamination of the CSF sample. This
is really bad
form. Do
not
cough into your sample. You and the patient went to a lot of
trouble--keep
it sterile.
- Disk herniation? There are rare
reports of disk
herniation
thought
to be caused by a previous LP that punctured an intervertebral disk.
- Impalement of nerve roots. Not likely
in a conscious
patient, who
will inform you quickly if he has lancinating pain shooting down one
leg.
It is more likely in an unconscious patient, so you may have to take
the
blame for it if the patient wakes up and finds he has a numb spot on
his
leg. But you may also get the credit for the patient waking up.
- Impalement of spinal cord. There is a
popular
misconception
that
paralysis is a possible complication of LP. This is not possible unless
you do a thoracic or cervical puncture because the spinal cord ends at
the L1/L2 disk. On the other hand, it is entirely
possible if
you
do C1/C2 punctures, or err during thoracic epidural anesthesia.
IV.
References
A good general review is:
Marra C.M. (editor), Central Nervous System Infections, Neurologic
Clinics
14, Philadelphia, W.B. Saunders & Co. (1999).
Specific references are:
1 Schachat, A., Robinson, K., Wenger, J.D. and et al., Bacterial
meningitis
in the United States in 1995, N Engl J Med, 337 (1997) 970
2 Progress toward eliminating Haemophilus
influenzae
type
b disease among infants and children--United States, 1987-1997, MMWR,
47
(1998) 993
3 Adams, W.G., Deaver, K.A., Cochi, S.L. and et al,
Decline of
childhood Haemophilus influenzae type b (Hib)
disease in the
Hib
vaccine era, JAMA, 269 (1993) 221
4 Murphy, T.V., White, K.E., Pastor, P. and et al.,
Declining
incidence of Haemophilus influenzae type b disease
since
introduction
of vaccination, JAMA, 269 (1993) 246
5 Mylonakis, E., Hohman, E.L. and Calderwood, S.B.,
Central
nervous
system infection with Listeria monocytogenes: 33
years'
experience
at a general hospital and review of 776 episodes from the literature,
Medicine
(Baltimore), 77 (1998) 313
6 Southwick, F.S. and Purich, D.L., Intracellular
pathogenesis
of listeriosis, N Engl J Med, 334 (1996) 770
7 Gray, B.M., Converse, G.M.D. and Dillon, H.C.J.,
Epidemiologic
studies of Streptococcus pneumoniae in infants, J
Infect Dis,
142
(1980) 923
8 Bishburg, E., Sunderam, G., Reichman, L.B. and et
al.,
Central
nervous system tuberculosis with the acquired immunodeficiency syndrome
and its related complex, Ann Intern Med, 105 (1986) 210
9 Cassleman, E.S., Hasso, A.N., Ashwal, S. and et
al.,
Computed
tomography of tuberculous meningitis in infants and children, J Comput
Assist Tomogr, 4 (1980) 211
10 Dooley, D.P., Carpenter, J.L. and Rademacher, S.,
Adjunctive
corticosteroid therapy for tuberculosis: a critical reappraisal of the
literature, Clin Infect Dis, 25 (1997) 872
11 Fodor, P.A., Levin, M.J., Weinberg, A. and et
al., Atypical
herpes simplex virus encephalitis diagnosed by PCR amplification of
viral
DNA from CSF, Neurology, 51 (1998) 554
12 Whitley, R.J., Kimberlin, D.W. and Roizman, B.,
Herpes
simplex
viruses, Clin Infect Dis, 26 (1998) 541
13 Carpenter, R.R. and Petersdorf, R.G., The
clinical spectrum
of bacterial infection, Am J Med, 33 (1962) 262
14 Dunbar, S.A., Eason, R.A., Musher, D.M. and et
al.,
Microscopic
examination and broth culture of cerebrospinal fluid in diagnosis of
meningitis,
J Clin Microbiol, 36 (1998) 1617
15 Atkinson, P.J., Sharland, M. and Maguire, H.,
Predominant
enteroviral
serotypes causing meningitis, Arch Dis Child, 78 (1998) 373
16 Gorgievski-Hrisoho, M., Schumacher, J.D.,
Vilimonovic, N.
and
et al., Detection by PCR of enterviruses in cerebrospinal fluid during
a summer outbreak of aseptic meningitis in Switzerland, J Clin
Microbiol,
36 (1998) 2408
17 McIntyre, P.B., Berkey, C.S., King, S.M. and et
al.,
Dexamethasone
as adjunctive therapy in bacterial meningitis: a meta-analysis of
randomized
clinical trials since 1998, JAMA, 278 (1997) 925
18 Sampathkumar P., West Nile Virus: Epidemiology, Clinical
Presentation,
Diagnosis, and Prevention, Mayo Clin Proc, 78 (2003) 1137-1144
19 de Gans J., van de Beek D. for the European Dexamethasone
in
Adulthood
Bacterial Meningitis Study Investigators, Dexamethasone in adults with
bacterial meningitis, N Engl J Med. 347 (2002) 1549-56.
20 Hanson R.A., Ghosh S., Gonzalez-Gomez I., Levy M.L., Gilles
F.H.
Abducens length and vulnerability? Neurology, 62 (2004) 33-36.
21 Kahn E.A., Cherry G.R. The clinical importance of
spontaneous
retinal venous pulsations. Univ Mich Med Bull 16 (1950) 305-398.
22 Cochlear implants may increase risk for bacterial
meningitis. Public Health Rep 119 (2004) 97-98.
23 Cohen N, Ramos A, Ramsden R, Baumgarten W, Lesisnski A,
O'donoghue G, Lenarz T, Fraysse B International consensus on meningitis
and cochlear implants. Acta Otolaryngol 125 (2005) 916-917.
24
Yogev R, Guzman-Cottrill J Bacterial meningitis in children:
critical review of current concepts. Drugs 65 (2005)
1097-1112.
25 Goldwater PN Cefotaxime and ceftriaxone
cerebrospinal fluid levels during treatment of bacterial meningitis in
children. Int J Antimicrob Agents 26 (2005) 408-411.
26 Antal EA, Loberg EM, Dietrichs E, Maehlen J
Neuropathological findings in 9 cases of listeria monocytogenes brain
stem encephalitis. Brain Pathol 15 (2005) 187-191.
27 Harrison LH Prospects for vaccine prevention of
meningococcal infection. Clin Microbiol Rev 19 (2006) 142-164.
28 Powers WJ Cerebrospinal fluid lymphocytosis in acute bacterial
meningitis. Am J Med. 792 (1985) 16-20.
V.
Quiz
Take a quiz! Test your knowledge of CNS infections. The quiz consists
of
25 questions.
First, let me know who you are, then click on the READY!
button to
start
the test.
This will open a new browser window.






